
Finally, in 1977, the company Minolta marketed the first pulse oximeter, which drove the market to improve oximetry technology. In fact, this technology is still used in today’s pulse oximeters. He had developed a pulse oximeter based on the ratio of red to infrared light absorption in blood (3). Then, in 1972, through the monumental work of Takuo Aoyagi, a Japanese bioengineer, oximetry finally became clinically feasible (2). In 1964, Hewlett Packard used eight wavelengths of light to further enhance the oximeter, however due to its size and cost, it was mainly used in sleep laboratories. A few years later, at Mayo Clinic, Wood had improved this device with the addition of an inflatable balloon to stop blood flow for calibration (1). In the 1940s, British scientist Millikan introduced the first aviation ear oximeter, which was used in pilot training in World War II. This was solved by the late 1930s by Squire, who created a self-calibrating oximeter. One of the main issues with this device was its difficult calibration. 70 years later, Matthes developed the first oxygen saturation meter, which used a 2-wavelength light source with red and green filters (1). Results: Pulse oximetry stems back to the 1860s, when hemoglobin was discovered to be the oxygen carrier in blood by Stokes. Objective: To review the evolution of pulse oximetry throughout history. It was not, however, invented overnight and there have been many stepwise monumental milestones that have led to the modern pulse oximeter that we all use today. The safety of anesthesia world-wide has been improved since its introduction. Kaminski: None.īackground: Pulse oximetry has been one of the most impactful innovations in anesthesia and critical care. Wayne State University School of Medicine, Detroit, Michigan, United Statesĭisclosures: W. 
There are no known risks or dangers of using a pulse oximeter when the values are reviewed and monitored by a competent health professional.Wenxi Gao, M.Sc., Edward R. Your doctor can clarify the significance of your value related to your particular situation. This saturation number (a good number would be over 90-92%) differs from a value called the pO2 (a good number would be over 60-65) which is measured by obtaining blood from an artery. The oxygen level may also help to determine if you need to receive supplemental oxygen. This number gives your doctors and nurses an idea of what your treatment will be. The measured amount shown on the screen reflects the saturation of your red blood cells with oxygen. The pulse oximeter observes a rapid measurement of oxygen saturation level in your body without using needles or taking a blood sample. By analyzing the light from the light source that passes through the finger, the device is able to determine the percentage of oxygen in the red blood cell. The pulse oximeter uses a cold light source that shines a light through the fingertip, making the tip appear to be red. 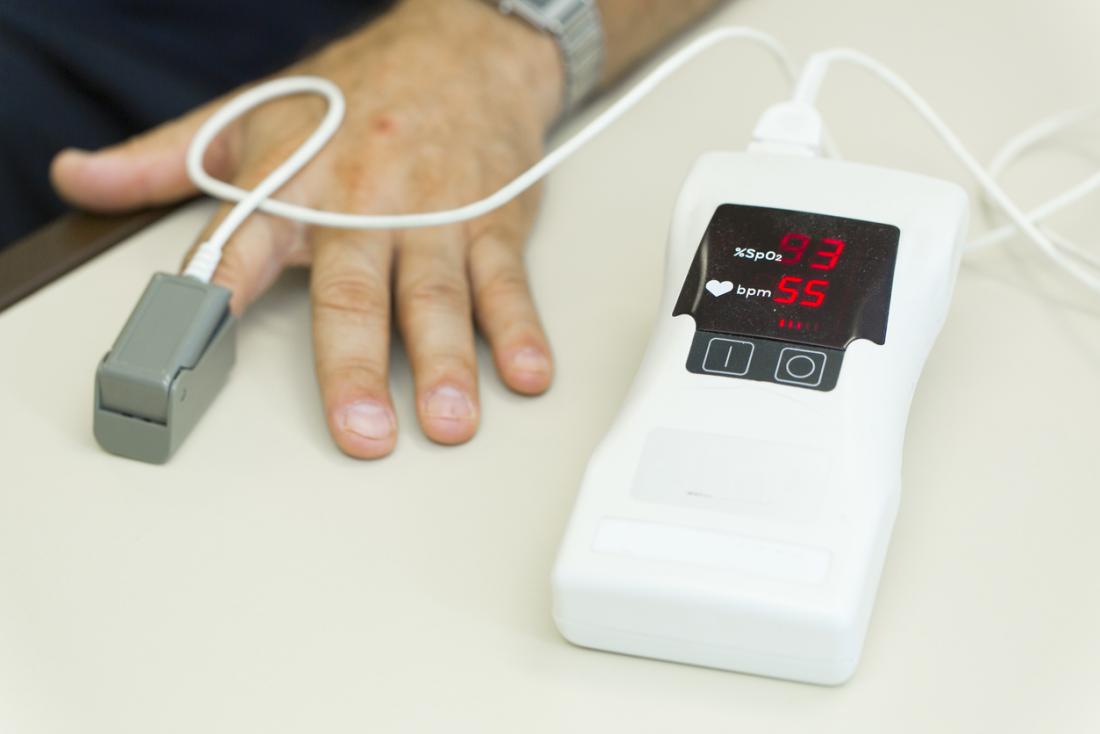
Some hospitals also use disposable tape probes that wrap around your finger, nose or toe. There are no needles and no pain involved in oximetry measurement. The probe will be positioned and within a few seconds, the oximeter will provide a readout of your heart rate and your oxygen saturation level, as in the picture above. If working accurately, you can expect a simple, quick and safe measure of the oxygen saturation level in your body. Read about COVID-19 and pulse oximetry in our Each Breath Blog: Pulse Oximetry – A Little Knowledge can be a Dangerous Thing. It is important to share readings that are abnormal or inconsistent with your healthcare provider. This is why the numbers from a pulse oximeter should not be used in isolation to determine your state of health. If you have poor circulation, dark skin pigmentation, thick skin, currently use tobacco, your skin temperature is cool, or you are wearing dark fingernail polish, long, artificial nails or if your fingers are not clean, the pulse oximeter may give inaccurate or inconsistent readings. In February 2021, the Food and Drug Administration issued an alert on limitations of pulse oximeters. If using this in a home setting, you should ask your healthcare provider before disposing of a pulse ox device, as it can be expensive and is reusable. 
The device may then be reused or disposed of. Pulse oximeters can be attached to your fingers, forehead, nose, foot, ears or toes. The pulse oximeter, or Pulse Ox, is an electronic device that measures the saturation of oxygen carried in your red blood cells. If you have a symptom of shortness of breath or a known lung or heart condition, your doctor may recommend use of a pulse oximeter.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
